


Find foods you can eat.
Introduction to an EoE Diet
Published on July 25, 2022If you have been diagnosed with Eosinophilic Esophagitis (EoE), you may be wondering what your treatment options may be. Since EoE can be triggered by food, one way to alleviate symptoms and identify your specific triggers is through diet! We’ve broken down the common EoE diets and how to follow them.
What is EoE?
Eosinophilic Esophagitis (EoE) is an immune condition that causes inflammation of the esophagus. In those with EoE, a type of white blood cell called eosinophils are found in excess in the lining of the esophagus thus causing inflammation. As a result, patients with EoE may have esophageal scars and experience trouble swallowing, persistent acid reflux, regurgitation, and chest pain. EoE is typically described as an allergic condition that is primarily provoked by foods in addition to environmental allergens and antibiotic use. Some individuals may also have a genetic predisposition for developing EoE.
Treatment Options for EoE
Recently, EoE has risen in prevalence throughout the United States; in fact, it is now the most commonly reported cause of dysphagia (or difficulty swallowing) in adolescents10. As cases and diagnoses of EoE have increased, so have the variety of treatment options. Currently, the most common treatments include medication, such as proton-pump inhibitors or steroids, and dietary therapy, which can take two forms: an elemental diet or an empirical elimination diet.
Medications are sometimes necessary to prevent or minimize permanent damage to the esophagus and abate inflammation. Forms of dietary elimination can achieve a reduction in inflammation and symptoms while also providing answers about a patient’s specific food triggers. This knowledge and insight about triggers of EoE provides patients with power and a sense of ownership over the condition. Furthermore, a diet-based approach is currently the only treatment option that aims to address the origin of EoE.6
EoE Diet Option 1: Elemental Diet
An elemental diet means that you only consume proteins in their most broken-down form: amino acids. The elemental diet has been shown to promote significant remission of EoE symptoms by removing any potential food allergens that may be triggering symptoms. 1, 5, 11 However, patients whose symptoms of EoE are triggered by environmental allergens instead of or in addition to certain foods will not respond to the elemental diet.
Although the elemental diet is a viable option for many patients (especially given the significant remission rates), it is highly restrictive and substantially disruptive to overall lifestyle. People who follow this diet consume an Amino acid-based formula (AAF)—a powder that can be mixed with liquids—in place of food. Some may receive AAF through a feeding tube instead of by mouth if they are unable to drink the volume of formula they require. The diet is also very expensive to follow as AAF is not covered by insurance in most states (insurance coverage by state can be found here). If choosing to follow an elemental diet, it is crucial to work with a registered dietitian (RD) to guide you and ensure that you are meeting your nutritional needs. 11
EoE Diet Option 2: Elimination Diet
The EoE elimination diet removes major food allergens that could trigger a patient’s symptoms. The traditional EoE elimination diet is a Six Food Elimination Diet (6FED or SFED). The six food groups eliminated in the 6FED are: dairy, wheat, egg, soy, nuts, and seafood; however, in the past decade, many researchers and physicians have been exploring alternative diets and variations to the classic SFED for treating EoE including step-up elimination diets.
Step-up Elimination Diets
In step-up elimination diets, patients first eliminate one or two of the most common triggers of EoE, and if symptoms and abnormal biopsies persist, the patient will eliminate the next most common triggers. As Lucendo and Molina-Infante’s article describes, step-up elimination diets “reduce the need for endoscopic procedures, shorten diagnostic process times, and avoid unnecessary restrictions.8” 1-3 FED, 2-4-6 FED, and 1-4-8 FED are a few step-up diets that have been explored.
Which EoE Diet should I follow?
(6FED, 1-3 FED, 2-4-6 FED, or 1-4-8 FED?)
Based on a review of relevant literature and counsel from Esophageal specialists at Duke University School of Medicine and University of North Carolina School of Medicine, the 2-4-6 Food Elimination Diet appears to be the most effective diet for reducing symptoms while also optimizing patient quality of life.3, 7, 8
This diet involves first cutting out the two most common triggers of EoE (dairy and wheat), followed by the next two most common triggers (soy and egg), and ending with the next two most common triggers (nuts and seafood). In addition to reducing endoscopic procedures by 20%, diets that eliminate the six EoE food groups have consistently resulted in roughly 72% remission. 1, 2, 8
How to approach the 2-4-6 Food Elimination Diet
Overview 2-4-6 FED
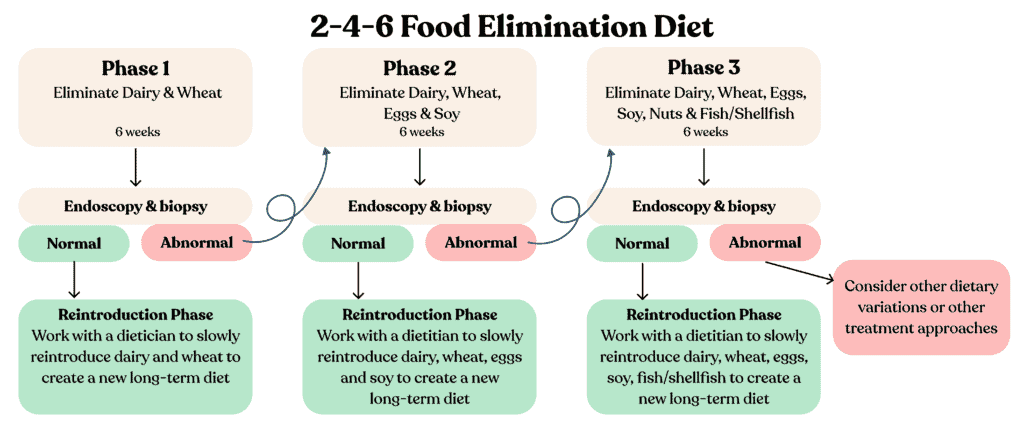
This framework can be easily adapted for other variations of EoE elimination diets, such as 1-3 FED and 1-4-8 FED.
Phase 1: Eliminate Dairy & Wheat (2-4-6 FED)
The first step in this 2-4-6 FED is the two-food elimination: cutting out dairy and wheat for six weeks. Dairy is by far the most common trigger found in 65-66% of patients9, 12. Wheat is the next most common trigger, found in roughly 27% of patients.9 In this step—as with every step of the elimination diet—careful attention to entirely cutting out all forms of dairy and wheat is crucial. Even a small amount would decrease the effectiveness of the FED. The Fig mobile app can help you identify dairy-free foods and navigate each part of the elimination diet, to aid you in catching less common or obscure forms of dairy and wheat.
After complete elimination of dairy and wheat for six weeks, the next step is to undergo an endoscopy. Unfortunately, solely relying on changes in symptoms is not an effective measure for determining if a certain food group is a trigger of your EoE symptoms or not, as it is possible to still have esophageal inflammation without experiencing significant symptoms. Instead, an endoscopy with biopsies is critical.
If your biopsy results are normal, your next step would be to meet with a dietitian to develop a plan for your future diet, while still maintaining balance and a high food quality of life. In other words, if there is a food you absolutely love, but it triggers your symptoms, dietitians can help you figure out how you can eat that food in different forms or different proportions. This process will involve slowly reintroducing foods and food groups to your diet as you become clearer on which foods/food groups specifically aggravate your EoE symptoms.
Phase 2: Eliminate Eggs & Soy (in addition to Dairy & Wheat) (2-4-6 FED)
If, however, after cutting out dairy and wheat your biopsies remained abnormal, it is recommended that you move onto the next part of the diet: four-food elimination. The additional two foods groups you would eliminate are the next two most common triggers of EoE: egg and soy (found to be triggers in 24% and 12% of patients, respectively9).
As you progress through the elimination diet, you must continue to cut out triggers from the previous elimination round. In other words, once you move on to the four-food elimination, you must continue to cut out dairy and wheat in addition to the two new food groups. This is because even if your biopsies were abnormal after cutting out dairy and wheat, your triggers may be dairy and another food group(s). Having more than one trigger occurs in more than half of patients with EoE.9
Phase 3: Eliminate Nuts & Seafood (in addition to Dairy, Wheat, Eggs & Soy) (2-4-6 FED)
The next steps will mimic the process after the first elimination round. If your symptoms persist and your biopsies remain abnormal, you will move onto the six-food elimination part of the diet, which includes cutting out nuts/tree nuts and fish/shellfish. If your symptoms do not persist and your biopsies return as normal, it is recommended that you work with a registered dietitian. They can assist in the food reintroduction process and make sure that you are not nutrient deficient (a common outcome in many EoE patients who do not properly manage their new diets).
Who should follow an EoE diet?
Some important questions to consider:
- What stage of life are you in right now?
- Do you have flexibility and control over the food you eat and where it comes from?
If for instance you are a college student on a meal plan, a diet-based approach to treating EoE may be quite difficult to navigate giving the confines of your university’s dining hall. If, however, you have the flexibility to cook for yourself, a diet-based approach may be a more viable option.
No matter what stage of life you are in, it is important to recognize the dedication and consistent hard work involved in a dietary-based treatment approach. That said, the additional knowledge about the root of your symptoms and food triggers that an elimination diet can provide is powerful.
Closing Thoughts on EoE Diets
The 2-4-6 FED diet has demonstrated high remission rates and is a streamlined approach to identifying EoE triggers. If you think the 2-4-6 FED diet is right for you, it is best to seek guidance from a physician or a registered dietitian.
Other EoE Diets: 1-4-8 FED & 1-3 FED
1-4-8 FED
A similar step-up diet that has been modeled (but lacks substantial data behind it like the 2-4-6 FED), is the 1-4-8 FED.
A collaboration between Harvard Medical School and University of North Carolina Medical School Chapel Hill in 2018 indicated that the 1-4-8 FED diet is the most effective diet at treating EoE, resulting in accurate determinations of food triggers for EoE in ~77% of patients.12 Although this slightly higher percentage (~77% compared to ~72% for the 2-4-6 FED) is appealing, it is generally advised that patients stick with the well-tested 2-4-6 FED until greater data on the 1-4-8 FED is available.
One notable advantage to the 1-4-8 FED, however, is that it eliminates corn and beef (in addition to nuts and shellfish). This is significant because there is a lack of consensus and conflicting data on what the next most common food group triggers are following dairy, wheat, soy, and eggs. Specifically, although many 2-4-6 FED elimination diets recommend nuts/tree nuts and fish/shellfish for the final set of eliminations, other studies have pointed to beef and corn as more common triggers of EoE. 12 That said, elimination of corn is highly restrictive (as it is found to be in a surprisingly wide range of foods), and thus can significantly lower overall quality of life when undergoing this part of the elimination diet.
1-3 FED
Another variation of the step-up diet that this collaboration between Harvard Medical School and University of North Carolina Medical School Chapel Hill explored is the 1-3 FED, which identified food triggers in 42.7% of patients. 12
Although this number is significantly lower than that of the 1-4-8 FED, the 1-3 FED is less disruptive to a patient’s life in terms of dietary restrictions and endoscopies. Specifically, patients who complete a 1-4-8 FED undergo an average of 4.13 endoscopies, while those on the 1-3 FED were found to undergo an average of 3.36 endoscopies. The number of endoscopies and required food groups to cut out are also important factors to consider when choosing an EoE diet. However, it is important to note that similar to the 1-4-8 FED, the 1-3 FED has much significantly less data behind it than the 2-4-6 FED.
The Fig Eosinophilic Esophagitis App can help you follow any of the above permutations of the EOE elimination diet.
As always, please consult with your own doctor or dietitian prior to starting any new diet and to determine the best course of action for your own health.
Special thanks to Julia Davis from Duke University for her significant contributions to this article.
Sources
- Arias, A., González-Cervera, J., Tenias, J. M., & Lucendo, A. J. (2014). Efficacy of dietary interventions for inducing histologic remission in patients with eosinophilic esophagitis: a systematic review and meta-analysis. Gastroenterology, 146(7), 1639–1648. https://doi.org/10.1053/j.gastro.2014.02.006
- González-Cervera, J., & Lucendo, A. J. (2016). Eosinophilic Esophagitis: An Evidence-Based Approach to Therapy. Journal of investigational allergology & clinical immunology, 26(1), 8–18.
- Goyal A. (2018). Eosinophilic esophagitis: short and long-term considerations. Current opinion in pediatrics, 30(5), 646–652. https://doi.org/10.1097/MOP.0000000000000662
- Groetch, M., Venter, C., Skypala, I., Vlieg-Boerstra, B., Grimshaw, K., Durban, R., Cassin, A., Henry, M., Kliewer, K., Kabbash, L., Atkins, D., Nowak-Węgrzyn, A., Holbreich, M., Chehade, M., & Eosinophilic Gastrointestinal Disorders Committee of the American Academy of Allergy, Asthma and Immunology (2017). Dietary Therapy and Nutrition Management of Eosinophilic Esophagitis: A Work Group Report of the American Academy of Allergy, Asthma, and Immunology. The journal of allergy and clinical immunology. In practice, 5(2), 312–324.e29. https://doi.org/10.1016/j.jaip.2016.12.026
- Liacouras, C. A., Spergel, J. M., Ruchelli, E., Verma, R., Mascarenhas, M., Semeao, E., Flick, J., Kelly, J., Brown-Whitehorn, T., Mamula, P., & Markowitz, J. E. (2005). Eosinophilic esophagitis: a 10-year experience in 381 children. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association, 3(12), 1198–1206. https://doi.org/10.1016/s1542-3565(05)00885-2
- Lucendo A. J. (2020). Nutritional approach to eosinophilic esophagitis: which diet and when. Minerva gastroenterologica e dietologica, 10.23736/S1121-421X.20.02797-X. Advance online publication. https://doi.org/10.23736/S1121-421X.20.02797-X
- Molina-Infante, J., Arias, Á., Alcedo, J., Garcia-Romero, R., Casabona-Frances, S., Prieto-Garcia, A., Modolell, I., Gonzalez-Cordero, P. L., Perez-Martinez, I., Martin-Lorente, J. L., Guarner-Argente, C., Masiques, M. L., Vila-Miravet, V., Garcia-Puig, R., Savarino, E., Sanchez-Vegazo, C. T., Santander, C., & Lucendo, A. J. (2018). Step-up empiric elimination diet for pediatric and adult eosinophilic esophagitis: The 2-4-6 study. The Journal of allergy and clinical immunology, 141(4), 1365–1372. https://doi.org/10.1016/j.jaci.2017.08.038
- Molina-Infante, J., & Lucendo, A. J. (2018). Dietary therapy for eosinophilic esophagitis. The Journal of allergy and clinical immunology, 142(1), 41–47. https://doi.org/10.1016/j.jaci.2018.02.028
- Spergel, J., & Aceves, S. S. (2018). Allergic components of eosinophilic esophagitis. The Journal of allergy and clinical immunology, 142(1), 1–8. https://doi.org/10.1016/j.jaci.2018.05.001
- Warners, M. J., Vlieg-Boerstra, B. J., & Bredenoord, A. J. (2015). Elimination and elemental diet therapy in eosinophilic oesophagitis. Best practice & research. Clinical gastroenterology, 29(5), 793–803. https://doi.org/10.1016/j.bpg.2015.06.013
- Warners, M. J., Vlieg-Boerstra, B. J., Verheij, J., van Rhijn, B. D., Van Ampting, M. T., Harthoorn, L. F., de Jonge, W. J., Smout, A. J., & Bredenoord, A. J. (2017). Elemental diet decreases inflammation and improves symptoms in adult eosinophilic esophagitis patients. Alimentary pharmacology & therapeutics, 45(6), 777–787. https://doi.org/10.1111/apt.13953
- Zhan, T., Ali, A., Choi, J. G., Lee, M., Leung, J., Dellon, E. S., Garber, J. J., & Hur, C. (2018). Model to Determine the Optimal Dietary Elimination Strategy for Treatment of Eosinophilic Esophagitis. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association, 16(11), 1730–1737.e2. https://doi.org/10.1016/j.cgh.2018.04.013
Photo by Philippe Gauthier via Unsplash.com
 What Exactly Are “Natural Flavors”?
What Exactly Are “Natural Flavors”? The Ultimate Guide to Sugars
The Ultimate Guide to Sugars